蔡卫华医生的科普号
- 精选 青年人颈椎病的临床特点及前路手术疗效观察
摘要:目的:探讨青年人颈椎病的临床特点、预防及前路手术效果。方法:回顾性研究2006年1月~2016年1月在江苏省人民医院骨脊柱病区进行前路手术治疗的48例年龄≤35岁的颈椎病患者。结合病史及影像学资料,分析该类患者的临床特点,通过比较术前、术后X片Cobb角及弓深变化,以及颈椎JOA评分、VAS评分来评估前路手术治疗效果。结果:脊髓型患者神经功能平均改善率为77.8±17.3%;神经根型患者术后VAS评分均为0.64±0.61分。Cobb角改善9.25±4.52°,弓深改善6.64±3.40mm,两种前路手术方式对神经功能恢复、弧度恢复及弓深恢复无影响,次全切失血量大,弓深改变与Cobb角改变有显著关系。随访半年以上患者均恢复工作。结论:青年颈椎病多发于长时间伏案工作或重体力劳动人群,颈椎曲度改变及椎间盘退变突出是主要致病因素,严重病例行颈前路手术安全有效,手术方式对结果无明显影响。本文系蔡卫华医生授权好大夫在线(www.haodf.com)发布,未经授权请勿转载。
蔡卫华 主任医师 江苏省人民医院 脊柱外科4564人已读 - 精选 急性颈脊髓损伤并发抗利尿激素分泌异常综合征蔡卫华 主任医师 江苏省人民医院 脊柱外科1456人已读
- 精选 原发性腰椎间隙感染的诊断和治疗
摘要:目的 分析原发性腰椎间隙感染的诊断及治疗。方法 2004 年8 月~2008年12月收治10例原发性椎间隙感染病例,男6 例,女4 例,年龄26~79 岁,平均52 岁。腰部剧烈疼痛7例,轻度腰痛3例,均有发热,体温37.8℃~40.0℃,平均38.3℃。有糖尿病史4例,病前前列腺有创检查2例、尿路感染2例。血常规白细胞计数6例无明显增高,4例感染扩散后出现白细胞计数增高;血沉48~120mm/h,平均60mm/h;C-反应蛋白55~98mg/L,平均72mg/L;术前血液和尿液培养阳性各1例,分别为金黄色葡萄球菌和大肠埃希杆菌。CT和MRI检查显示,L2/3和L3/4 1例,L4/5 4例,L5/S1 5例,CT检查发现相邻椎体边缘不规则骨质破坏9例,MRT1相病变椎间盘呈不均匀低信号影,MRT2相为均匀的高信号影9例,椎管内脓肿1例。3例症状轻的年轻患者保守治疗6周后症状消失,7例保守治疗3~4周无效后行手术治疗,3例后路植骨内固定+前路病灶清除术,2例前路病灶清除术植骨+前路内固定,1例单纯前路病灶清除术,1例后路病灶清除植骨+后路内固定术,术后继续保守治疗5~7周,手术病例均行病理检查。结果 早期5例误诊(3 例结核,2 例肿瘤)。随访18 个月,平均8 ~ 24个月。3 例保守治疗后腰痛症状缓解,治疗8 周后ESR 和CRP 恢复正常,X 线和CT 检查提示病变节段无脊柱不稳,终板破坏处出现硬化。7例术后病理均提示感染,术后2 ~ 5天腰痛减轻,2 周左右消失,2 ~ 3周后体温、ESR 和CRP 恢复正常。除1例术后6月邻近节段复发外,其他均在术后5月恢复正常生活和工作,植骨病例均骨性融合,平均融合时间3.4月(3~5月),无内固定松动和断裂。结论 原发性腰椎间隙感染临床症状缺乏特异性,早期易误诊。对症状轻的年轻患者,可保守治疗。对保守治疗无效者,手术治疗可能是本病有效安全的治疗方法之一。关键词: 腰椎;椎间隙感染;脊柱;内固定Diagnosis and treatment of spontaneous infectious discitis of lumbar spine. //CAI Wei-hua, ZHANG ning, JIN Zheng-shuai, HU Zhi-yi ,LIU Yong-ming CAO Xiao-jian, YIN Guo-yong. Department of Orthopaedics, the First Affiliated Hospital of Nanjing Medical University, Nanjing 210029,China.[Abstract ]Objective:To investigate the diagnosis and treatment of spontaneous infectious discitis of lumbar spine(SIDLS). Method:Clinical datas of ten cases of SIDLS treated from Aug 2004 to Dec 2008 were analysed. Male 6,female 4.Ages 26~79ys, mean 52ys.Seven cases had back severe spasm pain,3 cases had untypical back pain. All cases had fever range from 37.8℃ to 40.0℃ (average 38.3℃). History of past illness: diabetes mellitus 4 cases, invasive exam of prostate 2 cases, urinary tract infection 2 cases. Leucocyte number increased only in 4 cases after infection extension. Erythrocyte sedimentation rate ranged from 48mm/h to 120mm/h (average 60mm/h).C-reaction protein ranged from 55mg/L to 98mg/L (average 58mg/L). Two cases preoperative bacterial culture were positive in 2 cases ,one bacillus coli of blood, one staphylococcus aureus of urine. Involved level of CT and MRI: L2/3 combined L3/4 1 case,L4/5 4 cases,L5/S1 5 cases.CT exam displayed end plate irregular destruction of vicinity vertebras in 9 cases. MRI exam showed involved level uneven low signal changes in T1 phase, and well-distributed high signal changes in T2 phase in 9 cases, vertebral canal abscess in 1 case. Three young patients with slight pain were cured after conservative treatment for 6 weeks. Seven patients received operation after failed non-surgical treatment for 3 to 4 weeks, 3 cases anterior debridement with posterior instrumentation and bone graft, 2 cases anterior debridement and fusion with anterior instrumentation, 1case anterior debridement only because of old age, 1 case posterior debridement and interbody grafting with posterior instrumentation. Infection were certified by pathologic diagnosis in all cases. Conservative treatment was continued after operation for 5 to 7 weeks. Results Five patients were misdiagnosis at early stage(3 as tuberculosis, 2 as tumor). All cases were followed up from 8 to 24 months (average 18 months). Three conservative treated patients were cured after 8 weeks. Imageologic exam improved spine stabilization and end plate sclerosis of the initial erosion . Back pain , fever, ESR and CRP were relieved obviously of seven operated patients. Back pain disappeared within 2 weeks post-operation. Fever, ESR and CRP were normal from 2 to 3 weeks post-operation. All cases returned to normal life and work at 5 months post-operation, except 1 case recurred at vicinity vertebra after 6 months post-operation . All patients of bone graft obtained bone fusion within 5 months (average 3.4months). No implants loosening or breakage occurred. Conclusion Because of lacking specificity of its clinical manifestations, SIDLS is easy misdiagnosis on earlier period. Conservative treatment is effective for young patients without serious syndromes. Operation would be a effective and safe treatment in patients who had failed medical management.【Key words】lumbar ; disc space infection ;spinal column; internal fixation
蔡卫华 主任医师 江苏省人民医院 脊柱外科5725人已读 - 精选 下颈椎牵张屈曲型损伤手术入路的选择及疗效分析
【摘要】 目的 回顾性分析不同手术入路治疗下颈椎牵张屈曲型损伤的疗效。方法 回顾自2002年8月至2008年8月手术治疗的下颈椎牵张屈曲型损伤30例,根据不同类型、是否合并椎间盘损伤和术前牵引复位情况选择不同的手术方法。前路手术7例;后路手术5例;后路+前路手术11例;前路+后路+前路手术7例。分析相关指标:损伤节段Cobb 角及椎体水平移位的变化、神经功能恢复(Frankel 评分)、融合时间、融合率、手术时间以及并发症情况。结果 术后平均随访8个月(5~24个月),所有病例均获得骨性愈合,无内植物松动发生。Frankel 评分术前平均为1.67 分,术后平均2.22分。术前Cobb 角平均为7.78°,术后1.79°,水平位移术前平均3.67 mm ,术后恢复到0.53 mm。前后联合入路手术时间上较单纯前路或后路有明显差异,但在融合时间、Cobb 角、椎体水平移位、融合率和神经功能恢复、并发症等方面无明显统计学差异。结论 根据不同损伤情况选择不同手术入路治疗下颈椎牵张屈曲型损伤均可取得满意的疗效。手术入路的选择应根据关节突脱位、是否可以复位以及椎间盘损伤等情况综合考虑。【关键词】 颈椎;牵张屈曲型损伤;手术治疗;前路手术;后路手术Analysis of the choice of surgical approach and clinical results of distraction-flexion injury in the lower cervical spine. //CAI Wei-hua, ZHANG ning, LIU Yong-ming, HU Zhi-yi, YIN Guo-yong, CAO Xiao-jian,JIN Zheng-shuai . Department of Orthopaedics , The First Affiliated Hospital of Nanjing Medical University, Nanjing 210029, China.[Abstract] Objective To retrospective analysis of different surgical approach and its clinical results on the treatment of distraction-flexion injury in the lower cervical spine. Methods From Aug 2002 to Aug 2008, 30 cases with a distraction-flexion injury of the lower cervical spine were treated surgically. Seven cases were treated with anterior approach alone , 5 with posterior approach alone , 11 with posterior combined anterior approach and 7 were treated with a combined anterior - posterior - anterior approach. The following parameters were analyzed: the change of transverse displacement and Cobb’s angle, neurologic recovery(Frankel criteria),fusion time, fusion rate, surgery time, and the rate of complications. Results The mean following time was 8 months(5~24 m). Bone fusion reached in all patients. No plate and screw loosening occurred. The Frankel score increased from 1.67 preoperatively to 2.22 postoperatively. The Cobb’s angle was 7.78°before operation and 1.79°after operation , the transverse displacement was 3.67 mm before operation and 0.53 mm after operation. Combined anterior and posterior approach had a significantly longer mean operation time than anterior approach alone. There were no significant differences in the changes in fusion time, transverse displacement and Cobb’s angle, fusion rate, and neurologic recovery. Conclusions All the cases treated with different approach got satisfactory results. The determination of surgical approach should generally base on the condition of dislocation of facet joint ,reduction and injury of the disc.[Key words] cervical spine; distraction-flexion injury; operation; anterior approach; posterior approach
蔡卫华 主任医师 江苏省人民医院 脊柱外科2804人已读 - 医学科普 春节出行,安全第一!保护好颈椎,方能锦上添花
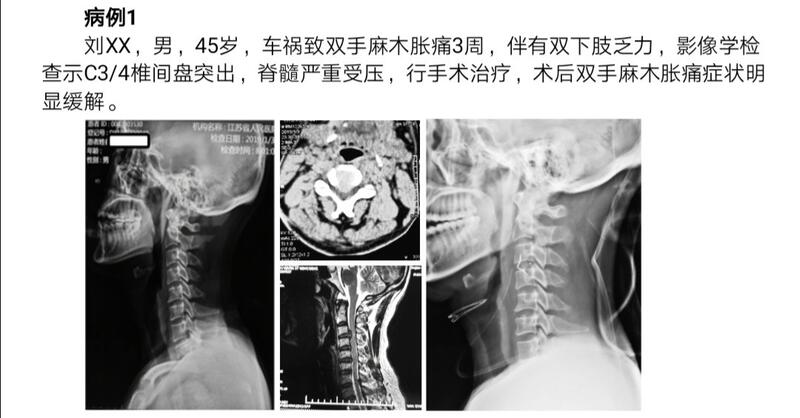
春节出行,保护好颈椎,才能锦上添花2019年春节就要到了,在这里提前给大家拜年,祝大家新年快乐诸事顺利!随着春节临近,开车返乡及出游人数逐年递增,越来越多的人选择自驾出行,但是如果平时有颈椎病或颈椎间盘突出症病史的人,那么在开车或坐车的时候需要格外注意,因为很有可能,这些人群就是汽车中的玻璃人。颈椎病是由于颈椎椎间盘退变后导致引起一系列的继发改变,如椎间盘突出、椎体后缘骨刺、钩椎关节增生,后纵韧带骨化、黄韧带肥厚或钙化,以此构成对脊髓或支配脊髓血管的压迫因素,导致不同程度的脊髓功能障碍的疾病。其中脊髓型颈椎病对患者伤害最严重,占全部颈椎病的10%~15%。脊髓型颈椎病发病过程中的机械因素可分为静态因素和动态因素。静态因素包括突出的椎间盘,后纵韧带骨化,椎体骨赘及增厚的黄韧带等,且椎管矢状径的绝对狭窄对脊髓型颈椎病的发病较为重要;动态因素包括正常和异常的运动及颈椎的负荷,可导致颈椎某节断不稳,此时以颈部局部症状为主。二者互为关系,导致椎体骨赘形成等静态因素的产生可抑制动力因素,减缓病情发展;动态因素得不到控制,静态因素不断增长,压迫脊髓导致脊髓型颈椎病的发生和发展。当静态因素已经形成,颈椎间盘突出,黄韧带骨化等均为导致颈椎管狭窄的因素,此时机体已然处于代偿状态,一旦再施加一个动态因素,如碰撞,追尾等车祸,骑车摔倒头面部着地,甚至是负重健身时不正确的动作,都有可能使病情突然加重,轻者造成双上肢麻木,乏力,握力下降;重者可导致四肢瘫痪乃至危机生命。年前我们治疗团队连续收到3例因轻微外伤导致严重脊髓损伤的患者,具体情况如下:病例1刘XX,男,45岁,车祸致双手麻木胀痛3周,伴有双下肢乏力,影像学检查示C3/4椎间盘突出,脊髓严重受压,行手术治疗,术后双手麻木胀痛症状明显缓解。 病例2房XX,男,64岁,车祸致双上肢麻木乏力疼痛3天,当时头房XX,男,64岁,车祸致双上肢麻木乏力疼痛3天,当时头面部着地,伤后即可四肢不能活动,数小时后双下肢逐步恢复力量,上肢近端肌力恢复,但残留双侧前臂痛觉过敏双手不能握紧,不能拿东西。影像学提示颈椎间盘突出(C3/4,C4/5,C5/6),颈3-5脊髓信号异常。手术彻底减压,术后患肢疼痛麻木及乏力即刻好转。 病例3张XX,男,45岁,平时有颈椎病病史,但担心手术风险,没有引起重视,年前在健身房做器械训练后突发四肢乏力,不能行走,误以为脑梗,入院时双下肢基本瘫痪,肌力0-1级,影像学提示颈椎间盘突出(C4/5,C5/6),后纵韧带骨化,手术行后路椎管减压,术后四肢肌力明显提高,目前在进一步康复治疗中。 脊髓型颈椎病主要临床表现为双侧或单侧下肢麻木、疼痛、僵硬脊髓型颈椎病主要临床表现为双侧或单侧下肢麻木、疼痛、僵硬发凉、发抖、无力、颤抖等症状,行走乏力,经常打软腿,易绊倒,有踩棉花、头重脚轻的感觉。之后会发展为双侧或单侧上肢麻木、酸胀、烧灼感、疼痛发抖、无力以及活动不灵活等,甚至不能做手执笔、握筷子、端碗、系扣子等精细动作。同时也可能出现胸腹部麻木、疼痛、有如捆绑的感觉。症状加重的同时,可能出现膀胱、直肠括约肌障碍,表现为尿急,一有想排尿的感觉便急不可耐,有时排尿控制不好甚至尿裤子,排尿无力、尿不尽感以及便秘等,严重者小便潴留或小便失禁。部分男性患者还可能有性功能障碍。尽管这三例患者经过及时有效的治疗后均取得满意疗效,在此我们友情提醒大家,如果平时出现颈部疼痛,四肢麻木乏力,行走不稳等,建议在节假日最好避免长途驾车或坐车,尽量避免到人群拥挤的地方,同时在坐车或骑车时可能做好防护措施,并且保持注意力集中,避免摔倒,最大程度的防止碰撞。如果是健身爱好者,在负重锻炼前需要专业脊柱外科医生指导,以免在锻炼过程中加重病情,适得其反,造成不可挽回的伤害。 蔡卫华,男,南京医科大学第一附属医院(江苏省人民医院)脊柱外科,主任医师,教授,医学博士,博导。临床方向:颈椎、腰椎退变性疾患的诊治,如颈椎病、颈椎管狭窄症、颈椎创伤、腰椎间盘突出症、腰椎管狭窄症、腰椎不稳、腰椎退变性侧凸等。2011/11-2012/02在美国Thomas Jefferson University进行学术交流;2014/10在法国斯特拉斯堡大学医院学习颈椎腰椎人工椎间盘置换。科研方向:脊髓损伤的基础研究。获江苏省六大人才高峰资助项目1项,江苏省333第三层次培养和资助对象,主持国家自然科学基金面上项目2项,江苏省自然科学基金面上项目1项,主要参与国家自然科学基金项目3项,发表论文30余篇,SCI 12篇。社会兼职美国国际脊柱新技术学会(ISASS) 会员中国康复医学会脊柱脊髓专委会颈椎研究学组 委员中国医药教育协会骨科专业委员会南京培训基地 副主任委员兼秘书长中国残疾人康复协会肢体残疾康复专业委员会脊柱康复学组 常委江苏省中西医结合学会脊柱医学专业委员会 常委江苏省康复医学会修复与重建委员会 常委中国医药教育协会骨科专业委员会脊柱分会 委员江苏省康复医学会脊柱脊髓专业委员会颈椎学组 副主任委员
 蔡卫华 主任医师 江苏省人民医院 脊柱外科1人已购买
蔡卫华 主任医师 江苏省人民医院 脊柱外科1人已购买 - 引用 椎间盘突出为什么做完了X光片、CT还要做磁共振MRI?
首先X光片不能作为确诊椎间盘突出症的证据,但可排除结核、肿瘤、椎体滑脱等疾病,并初步判断脊柱的形态,稳定和退变程度。CT显示骨性结构上有优势,可显示小关节增生肥厚、椎管及侧隐窝狭窄等情况,但CT对软组织如椎间盘显示不如MRI。MRI大多情况下都优于CT,特别是在椎间盘、感染和肿瘤的诊断上,能清楚地显示椎间盘的类型和脊髓受压程度。但在显示骨皮质、钙化或骨化组织又不如CT。实际上三者是互补的,可有效降低误诊率。但由于MRI检查的时间一般需20~30分钟,预约时间较长,而且MRI机器昂贵并非所有医院都具备,所以应用最多的是CT。但如果症状严重,需行手术,诊断必须清楚!所以术前X光片、CT和MRI都是必不可少的!本文系凌钦杰医生授权好大夫在线(www.haodf.com)发布,未经授权请勿转载。
凌钦杰 主治医师 广医一院 脊柱外科9672人已读 - 引用 颈部及腰背肌锻炼(颈椎、腰椎保健操,原创)
门诊很多病人出现颈部、腰部及腿部的疼痛,大多数患者都是因为颈部及腰背部肌肉痉挛造成的,本文提供了颈部及腰背部肌肉的功能锻炼,对于出现在早期的患者有很好的指导意义。大家按照图示要求进行锻炼,坚持下去,会收到很好的效果。(贵在坚持,务必坚持!)颈椎、腰椎保健操,颈椎、腰椎保健操,颈椎、腰椎保健操,颈椎、腰椎保健操,颈椎、腰椎保健操
郑帅 副主任医师 南方医科大学南方医院 脊柱骨科4.2万人已读 - 引用 锻炼颈、胸、腰背肌的方法:小燕飞 或 蛙泳
适用于:腰肌劳损、腰肌筋膜炎、腰椎间盘突出症、腰椎峡部裂、轻度腰椎滑脱、腰椎术后。颈椎、胸椎患者也可以锻炼,小燕飞可以锻炼整个背部肌肉(颈椎+胸椎+腰椎)。最好是终生锻炼。小燕飞的方法是:头和胸部抬起
姜亮 主任医师 北医三院 骨科23.3万人已读





